A mammogram screening is a specialized X-ray test designed to spot breast cancer in its earliest stages, often before any symptoms appear. Unlike a regular check-up or breast exam, this imaging test uses low-dose radiation to create detailed pictures of the breast tissue. These images help doctors identify subtle changes, such as tiny calcium deposits (microcalcifications) or small tumors that are too deep or too small to feel. Mammogram Screening (2025)
There are two main types of mammography. A screening mammogram is performed on women who have no breast symptoms—it’s a routine preventive tool. On the other hand, a diagnostic mammogram is used if there’s a lump, pain, or an abnormal result from a screening test. While both use the same imaging technology, the diagnostic version includes more detailed views to pinpoint specific areas of concern.
During mammogram screening, the breast is gently compressed between two plates while X-ray images are taken. Compression might sound uncomfortable, but it only lasts a few seconds and is crucial for producing clearer images while lowering radiation exposure.
Why Mammogram Screening Matters: Benefits & Limitations
The biggest advantage of mammogram screening is its ability to catch breast cancer early, often years before it can be felt as a lump. Early detection means more treatment options, less invasive procedures, and a much higher chance of survival. In fact, studies consistently show that women who undergo regular mammography have a lower risk of dying from breast cancer compared to those who don’t.
Another important benefit is reassurance. A normal screening mammogram result can give peace of mind, especially for women with a family history of breast cancer. For those with dense breasts, mammography can highlight areas that need closer attention and guide whether additional tests, such as ultrasound or MRI, are needed.
That said, no test is perfect. Mammogram screening sometimes produces false positives—results that suggest cancer when none is present. This can lead to extra imaging or even a biopsy, which may cause stress and added costs. On the other side, false negatives are possible, meaning a cancer could be missed, especially in very dense breast tissue. Overdiagnosis is another limitation; some cancers found may never have caused harm, yet treatment still follows.
Mammogram Screening Guidelines 2025
One of the most common questions women ask is: When should I begin mammogram screening? The answer depends on your personal risk factors, but several respected organizations have issued updated guidelines for 2025.
For average-risk women, most experts recommend starting mammogram screening at age 40. The American College of Obstetricians and Gynecologists (ACOG) and the American Cancer Society (ACS) recommend that women aged 40 to 44 may opt for annual screening, while those aged 45 to 54 should undergo a mammogram annually. From age 55 onward, screening can be continued every one to two years as long as the woman remains in good health.
The U.S. Preventive Services Task Force (USPSTF) recently updated its guidance as well, advising biennial screening for women ages 40 to 74. This marks a shift from earlier recommendations, reflecting growing evidence that starting earlier saves more lives.
For women at higher risk, screening usually begins earlier—sometimes as young as 30. This group includes those with a strong family history of breast cancer, inherited gene mutations such as BRCA1 or BRCA2, or a history of chest radiation therapy. In addition to mammography, doctors often recommend an annual breast MRI to improve detection rates.
Special groups also need tailored guidance. Men with breast symptoms should not ignore them and may be advised to undergo diagnostic mammography. Transgender women on long-term hormone therapy and transgender men who have not had chest surgery should also discuss individualized screening plans with their health-care provider.
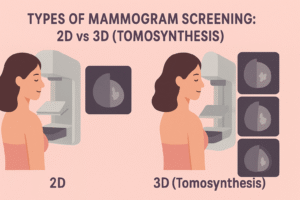
Types of Mammogram Screening: 2D vs 3D (Tomosynthesis)
Not all mammogram screenings are the same. Today, women typically have two main options: 2D digital mammography and 3D mammography, also called digital breast tomosynthesis. Understanding the difference helps you make an informed choice.
A 2D mammogram creates two flat images of each breast—one from the top and one from the side. This has been the standard method for decades and remains highly effective at detecting many forms of breast cancer.
A 3D mammogram screening goes a step further. Instead of taking just two images, the machine captures multiple slices of the breast from different angles. A computer then reconstructs these into a layered, three-dimensional image. This makes it easier for radiologists to see through overlapping tissue, which is especially valuable for women with dense breasts.
Research shows that 3D mammography can reduce the number of callbacks (when patients are asked to return for more imaging) and may improve cancer detection rates. However, availability and insurance coverage vary. Some facilities charge extra for 3D, while others include it in routine screening.
Both methods use low-dose X-rays and are considered safe. If you’re uncertain which option is right for you, ask your doctor whether 3D mammogram screening is available in your area and whether it offers advantages based on your breast density or medical history.
Mammogram Screening vs. Other Imaging Tests
While mammogram screening is the gold standard for early breast cancer detection, other imaging tools also play an important role. Understanding how they compare helps patients know what to expect if additional tests are recommended.
A breast ultrasound uses sound waves to produce images of breast tissue. It’s especially useful for investigating a lump felt during an exam or for women with dense breasts, where mammograms may not capture the full picture. Ultrasound is often used as a follow-up test, not a replacement for a screening mammogram.
A breast MRI (magnetic resonance imaging) offers even more detail, using magnets and radio waves instead of radiation. It’s highly sensitive and often recommended for women at high risk, such as those with BRCA gene mutations or a strong family history. However, MRI tends to pick up more false positives, which can lead to extra testing.
Compared to these tools, mammogram screening remains the first-line choice for most women because it is widely available, quick, cost-effective, and supported by decades of research. Ultrasound and MRI are valuable additions in specific cases, but they don’t replace the proven benefits of routine mammography.
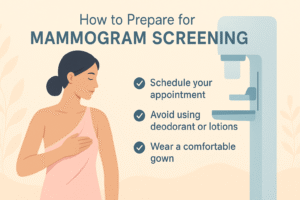
How to Prepare for Mammogram Screening
Good preparation can make your mammogram screening smoother and more comfortable. A few simple steps will help ensure the clearest images and reduce stress on the day of your appointment.
Avoid deodorants, lotions, or powders on your chest and underarms before the test. These products can leave tiny particles on the skin that may appear as white spots on the X-ray, interfering with your results.
Schedule wisely. If you’re premenopausal, try to book your screening mammogram a week after your period, when your breasts are less likely to feel tender. This can help reduce discomfort during the brief compression.
Bring past mammogram results if you’re going to a new facility. Comparing current images with older ones allows the radiologist to spot subtle changes more accurately.
During the procedure, you’ll be asked to undress from the waist up and wear a gown. Each breast will be positioned on the imaging plate, gently compressed, and X-rayed from a few angles. The compression lasts only a few seconds but is essential for producing clear images with the lowest possible radiation dose.
If you have breast implants, dense breasts, or previous surgeries, let the technologist know. Special techniques can be used to capture better images.
Overall, preparation is simple, but it makes a big difference. With the right steps, your mammogram screening will be quicker, more accurate, and less uncomfortable.
Understanding Mammogram Screening Results
After your mammogram screening, the images are reviewed by a radiologist who looks for signs of unusual changes in breast tissue. Your results are usually reported using the BI-RADS system (Breast Imaging Reporting and Data System), which provides a clear framework for interpretation.
BI-RADS 0: Incomplete; more images are needed.
BI-RADS 1–2: Negative or benign, meaning no signs of cancer.
3: Probably benign, but a short-term follow-up may be recommended.
4–5: Suspicious or highly suggestive of cancer, often leading to a biopsy.
In some cases, women are asked to return for additional imaging. This recall doesn’t automatically mean cancer is present—it often means the radiologist wants a closer look at an area that wasn’t clear in the first screening. Follow-up may include diagnostic mammography, ultrasound, or even MRI.
If a biopsy is recommended, it involves removing a small tissue sample for lab testing. While hearing this news can be stressful, keep in mind that many biopsies turn out to be non-cancerous.
Most women receive results within a few days to a week. Whether your outcome is normal or requires follow-up, understanding the BI-RADS categories helps you feel more informed and confident about your next steps.
Risks & Safety of Mammogram Screening
One of the most common concerns about mammogram screening is radiation exposure. The good news is that the dose is very low—roughly equal to what you’d get from flying cross-country. For most women, the benefits of early breast cancer detection far outweigh this minimal risk.
Other potential risks include false positives, which may lead to follow-up imaging or a biopsy, and false negatives, where a cancer could be missed. These limitations are why consistency matters: repeated screenings over time increase the likelihood of finding abnormalities early.
For women with breast implants, technologists can use special views to capture clearer images. If you’re pregnant or breastfeeding, mammogram screening may be delayed or modified, since breast tissue can appear denser and more sensitive during this time. In such cases, your doctor may suggest an ultrasound instead.
It’s also worth noting that mammograms can occasionally cause anxiety due to recalls or additional testing. While this can be stressful, most follow-up results turn out to be benign.
Overall, mammogram screening is considered safe, quick, and effective. With its ability to save lives by catching cancer early, the advantages strongly outweigh the potential downsides.
Special Considerations in Mammogram Screening
While mammogram screening is useful for most women, certain situations call for tailored approaches.
Dense Breasts
Women with dense breast tissue have less fatty tissue and more glandular tissue, which can make it harder for X-rays to detect small cancers. Dense tissue may also increase the risk of breast cancer itself. In these cases, doctors may recommend supplemental imaging such as an ultrasound or an MRI alongside routine screening mammograms.
Breast Implants
If you have breast implants, it’s important to let your technologist know before the exam. Implants can obscure part of the breast tissue, so special displacement views are taken to allow better visualization. Mammogram screening is still safe, but the process may take slightly longer.
Men and Transgender Patients
Although breast cancer is less common in men, it does occur. Men with symptoms such as lumps or nipple changes may be referred for a diagnostic mammogram. Transgender women on hormone therapy and transgender men who haven’t had chest surgery should also discuss individualized screening schedules with their healthcare provider, since hormone use and breast tissue development affect risk levels.
In all these cases, the key is communication. Let your care team know about implants, prior surgeries, or unique circumstances so your mammogram screening can be as effective and accurate as possible.
Cost & Coverage of Mammogram Screening
The cost of mammogram screening can vary depending on where you live, the type of facility, and whether additional imaging is needed. On average, in the United States, a screening mammogram may cost between $100 and $250 without insurance. Diagnostic mammograms, which take more images and may involve additional tests, can be more expensive.
Fortunately, many insurance plans, including Medicare and Medicaid, cover the full cost of routine screening mammograms for women in the recommended age groups. The Affordable Care Act (ACA) requires most private insurers to provide coverage for screening every 1–2 years without out-of-pocket costs. If you’re uninsured, community health programs and nonprofit organizations sometimes offer free or low-cost mammogram screenings.
Coverage for supplemental imaging, such as ultrasound or MR, varies. If you have dense breasts, a family history of cancer, or a genetic predisposition, your doctor may recommend these additional tests. Some states now require insurance companies to cover them, but it’s best to check with your provider beforehand.
The bottom line: cost should never prevent you from getting screened. Early detection not only saves lives but can also reduce long-term treatment expenses. If affordability is a concern, ask your healthcare provider about local programs or financial assistance options. Mammogram Screening (2025)
Myths & Facts About Mammogram Screening
There are many misconceptions about mammogram screening, and separating myth from fact can help women make informed choices.
1 Myth: Mammograms cause cancer because of radiation.
Fact: The radiation from a mammogram is extremely low—similar to what you’d be exposed to during a cross-country flight. The benefits of early detection far outweigh this minimal risk.
2 Myth: Mammogram screening is only necessary if you have symptoms.
Fact: Breast cancer often develops silently in its early stages. Screening can detect changes long before a lump is felt or symptoms appear.
3 Myth: A clear mammogram means you’ll never get breast cancer.
Fact: While mammograms are highly effective, they aren’t perfect. Regular screenings, combined with self-awareness and clinical exams, provide the best defense.
Myth 4: Mammogram screening is too painful.
Fact: Compression can be uncomfortable, but it lasts only a few seconds. For most women, the procedure is tolerable and well worth the peace of mind it provides.
By understanding these facts, women can approach mammogram screening with confidence, knowing it’s one of the most reliable tools for protecting breast health. Mammogram Screening (2025)

Conclusion: Prioritizing Your Health with Mammogram Screening
Mammogram screening is one of the most powerful tools available for protecting women’s health. Detecting breast cancer early dramatically improves the chances of successful treatment and recovery. While it’s natural to have concerns about cost, discomfort, or radiation exposure, the facts show that screening is safe, widely accessible, and life-saving.
Every woman’s health journey is unique, and so are the recommendations for when and how often to screen. Talking with your healthcare provider about your personal risk factors—such as age, family history, or genetic predispositions—can help you create the right plan for your breast health. Mammogram Screening (2025)
FAQ:
- At what age should I start mammogram screening?
Most guidelines recommend beginning mammogram screening at age 40and continuing every 1–2 years. Women with a strong family history or genetic risk (such as BRCA mutations) may need to start earlier, often at age 30, after discussing with their doctor. - How often should I get a mammogram?
For women at average risk, once every 1–2 years is typical. High-risk women may need annual screenings, sometimes with supplemental imaging like MRI or ultrasound. - Does a mammogram hurt?
You may feel some pressure or discomfort when the breast is compressed, but it usually lasts only a few seconds. Most women describe the experience as tolerable rather than painful. - What if my mammogram shows something abnormal?
An abnormal result doesn’t always mean cancer. It could indicate a cyst, calcification, or benign growth. In such cases, your doctor may recommend additional imaging or a biopsy to confirm the findings. - Can I get a mammogram if I have breast implants?
Yes. Special displacement techniques are used to ensure clear imaging of breast tissue. It’s important to inform your technologist about your implants before the procedure.

